November is pancreatic cancer awareness month, when health care professionals call attention to a disease that affects more than 55,000 people in the United States each year. Pancreatic cancer is an especially deadly cancer because of the way it silently spreads before being detected.
Pancreatic cancer accounts for about 3% of all cancers in the United States and about 7% of all cancer deaths. The disease is ranked as the 14th most common cancer and the 7th deadliest cancer worldwide. Pancreatic cancer is difficult to diagnose because symptoms are not obvious during early stages, many symptoms are common to other conditions, and because examining the pancreas is not easy.
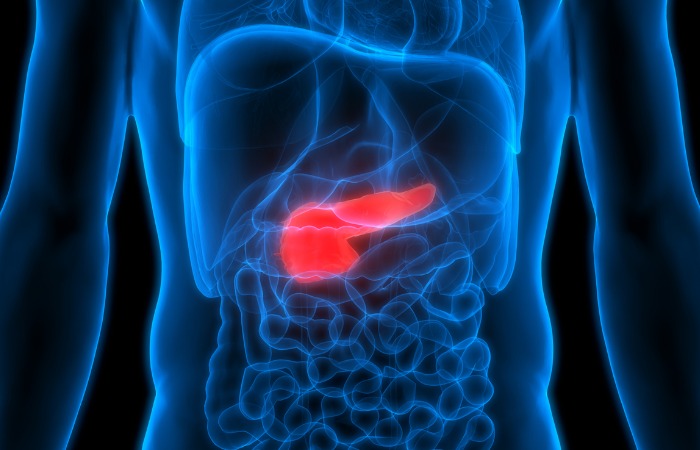
Pancreatic cancer originates just behind the stomach in the pancreas, a small organ that helps with digestion and controls the amount of sugar in the blood. There are two types of pancreatic cancer tumors: pancreatic adenocarcinoma tumors and pancreatic neuroendocrine tumors.
Pancreatic adenocarcinoma tumors are the more common form. Nearly 54,000 people in the United States are diagnosed with them each year, or about 1 in every 62 adults. Pancreatic neuroendocrine tumors are less common, but they are being seen more often in recent times. The treatment for each type varies. Treating pancreatic neuroendocrine tumors is a complex process, but it in some cases it can be cured.
Risk Factors and Symptoms
The average lifetime risk of pancreatic cancer is about 1 in 64. Certain health conditions can affect those odds. Some of the key risk factors are highlighted below:
- Smoking is one of the biggest risk factors for pancreatic cancer. The risk is about twice as high among smokers compared to those who never smoked.
- Obesity
- Personal history of diabetes, especially in people with type 2 diabetes. It’s not clear if people with type 1 diabetes have a higher risk.
- Family history of pancreatic cancer or pancreatitis
- Inherited genetic syndromes, such as hereditary breast and ovarian cancer syndrome (HBOC) or familial atypical multiple mole melanoma (FAMMM) syndrome
Easily detectable signs or symptoms usually are not present during the early stages of the disease. Even when present, they may be similar – if not identical – to symptoms of other conditions. Symptoms include:
- Jaundice (yellowing of the skin and whites of the eyes)
- Light-colored stools (clay-colored)
- Dark urine (like Coca-Cola)
- Pain in the upper or middle abdomen and back
- Unexplained weight loss
- Loss of appetite
- Fatigue
Diagnosis
Pancreatic cancer usually is diagnosed with tests and procedures that make pictures of the pancreas and the area around it. Examining the pancreas is not easy because it is located deep behind the stomach, small intestine, liver, gallbladder, spleen, and bile ducts. There are many types of imaging methods used for diagnosis, such as CT scans, MRIs, and X-rays. Images and tests are used before and after a diagnosis of pancreatic cancer to see how far the cancer may have spread, to determine if treatment is working, and to look for signs of cancer coming back after treatment.
For anyone who needs pancreatic care, UAB Medicine features experienced specialists, the most advanced technology, and in some cases medications and other treatments being evaluated in clinical research trials that are not available at most other medical centers. These resources are combined in UAB’s Pancreatobiliary Disease Center, which provides advanced care for pancreatic, bile duct, and gallbladder cancers.
Click here to learn more about pancreatic cancer diagnosis and treatment at UAB Medicine.
American Cancer Society: Cancer Facts and Figures 2020. Atlanta, Ga: American Cancer Society, 2020
National Center for Biotechnology Information, U.S. National Library of Medicine
